Sacro-Iliac Dysfunction
Key Sacro-Iliac facts you need to know.
SACRO-ILIAC DYSFUNCTION
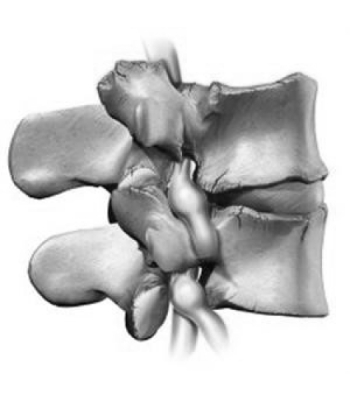
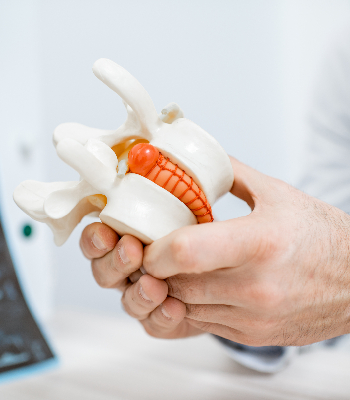
The sacroiliac joint is located in the buttock on each side and takes its name from the two bones which form the joint – the Sacrum (which is an upside-down triangular bone at the base of the spine) and the two iliac bones which when joined together form the pelvis.
It’s an unusual joint because it doesn’t allow a lot of motion and because the shape of the joint surfaces are quite irregular with an undulating, wavy joint surface (Most other joint surfaces are smooth).
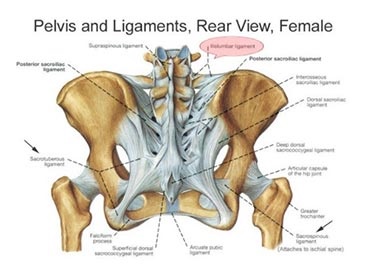
Because of its location all the upper bodyweight is placed upon it and when the foot strikes ground all of the bodyweight is transmitted to alternating sides of the joint with each stride. In order to support this a strong series of ligaments are attached around the sacroiliac joint and are shown left:
These ligaments are reinforced by many of the muscles around the lower back, buttock, abdomen and even the groin. Yes this is “The Core” plus a lot more as many muscles control this region. These muscles include the lower back, buttock, abdomen and even the groin. Yes this is “The Core” plus a lot more!

Biomechanics
All movements of the lower spine and legs produce some small motions of the sacroiliac joint. What this really means is that the lumbar spine, sacroiliac joints and hips work together as a functional unit. In practice, this means that if one part of this system is not functioning properly it has consequences for the other. In clinic we frequently see sacroiliac pain as a secondary consequence of stiffness in the lumbar spine or because of loss of motion and hip. It is very important to address these findings when present in order to unload the irritated sacroiliac joint and restore normal function.
When we bending forwards the lumbar spine flexes, the sacroiliac joint tips forwards between the pelvic bones and the pelvis rotates forwards on the ball-and-socket of the hips. Disturbances in these mechanics frequently cause sacroiliac joint pain. Another common trigger for sacroiliac pain occurs when putting on shoes & socks which combines the forward bending of the lumbar spine together with the flexing of the hip which can stress the sacroiliac ligaments from the top and bottom.
Symptoms
Because the sacroiliac joint has a lot of different nerves supplying it, pain originating from the joint can be quite variable. Most commonly it is specifically in the buttock usually along the joint line and below the waist which helps to differentiate it from the lumbar spine. Sometimes pain can be referred further down the leg – this is referred pain not radicular from nerve entrapment. Frequently when the sacroiliac joint is irritated there is secondary muscle spasm around the buttock muscles and disturbance of hip joint mechanics which can often cause pinching/ in the groin and can easily be confused with a primary hip joint problem.
In a small proportion of cases symptoms can present like sciatica but the key differentiating factor here is that the lumbar spine appears normal on examination/investigation. When this is the case the sciatic nerve can be irritated as it passes underneath one of the muscles of the sacroiliac joint known as Piriformis. This condition is known as Piriformis Syndrome. The piriformis muscle together with some other muscles in the buttock frequently go into spasm when the joint is irritated and nerve irritation is the result in a small proportion of people.
Frequently symptoms will alternate from one sacroiliac joint to the other with the resultant pain pattern that switches sides. This can initially appear alarming but, as can be seen from the discussion on mechanics, the sacroiliac joint moves on both sides simultaneously and therefore a disturbance on one side has direct consequences for its partner.
Causes
Until the late 1930s, low back pain was generally attributed to sacroiliac joint dysfunction. Around that time the discs in the lumbar spine became the focus of attention and since then much low back pain is attributed to “disc problems”. The best research estimates suggest that about 30% of chronic low back pain originates primarily from the sacroiliac joint – so that’s a significant number of people!
Pregnancy
traditionally pregnancy is the most widely recognised condition associated with sacroiliac pain. This is usually attributed to the softening of the ligaments which occurs in the later stages of pregnancy in order to allow the pelvic joints change position for childbirth. It is also associated with the change in spinal alignment as the “bump” gets bigger, and the subsequent change in muscle activity as the size and shape of the abdomen and pelvis change. Unfortunately, a significant number of women have ongoing persistency sacroiliac joint pain after pregnancy and unfortunately it is often poorly managed a recognised.
Spinal scoliosis
asymmetrical lateral curvature of the spine can result in overloading of one of the sacroiliac joints.
Trauma
falls onto the buttocks, slipping or jarring the leg on steps are typical mechanism’s to cause irritation of the sacroiliac joint.
Road traffic accidents
are another cause of sacroiliac dysfunction as a result of impact to the leg when braking and the upper body being pushed forward and impact.

Congenital hip dysplasia
by virtue of the disturbance in normal hip mechanics and alignment sacroiliac joint is frequently involved secondary to this.
Treatment
The first priority in treating sacroiliac joint dysfunction is to re-align the joint and reduce sensitivity of the surrounding sore tissues. There are quite a selection of corrective techniques and therefore vitally important that skilled assessment determines appropriate selection . These manipulative techniques are usually supplemented with soft tissue work to the surrounding musculature with a view to restoring range of movement, reducing muscle spasm and eliminating tender trigger points within the muscles.
In some cases, particularly pregnancy, a pelvic stabilisation belt may be required in order to maintain the position of the pelvic joints particularly when the ligaments have become more elastic and the muscle tone has switched off.
One key factor in preventing recurrence is to re-coordinate the musculature around the lumbar spine, pelvis and abdomen in order to ensure correct muscle activation to support the joints whilst allowing normal daily movements. Although core exercises are commonly prescribed there is usually a more intricate process of evaluation to identify specific muscle dysfunction and ensure a coordinated return to function. This requires a skilled physiotherapy evaluation with a precise treatment plan to maximise recovery.
BACK PAIN – SPECIFIC CONDITIONS
JOIN OUR MAILING LIST
EMAIL: